
Open enrollment for 2026 marketplace coverage officially started on November 1, 2025, and will run through January 15, 2026. We are already hearing from Arkansans whose premiums are jumping – in some cases, by hundreds of dollars a month. If you buy your own insurance through Healthcare.gov, this year is different in several important ways, and it is worth taking the time to look closely at your options.
Below is a rundown of what is happening, what changed because of H.R. 1 (AKA the “One Big Beautiful Bill”), and what people can be doing now to protect their coverage.
Why This Open Enrollment Matters More Than Usual
The Affordable Care Act marketplace is how more than 22 million people across the country get coverage, including tens of thousands in Arkansas. Almost everyone who buys a marketplace plan (93%) gets financial help called a premium tax credit enhancement to bring down monthly costs.
Those extra savings, which began in 2021 and drove record marketplace enrollment, are scheduled to end after 2025. Congress did not extend them in H.R. 1. This means the cost of coverage will rise sharply next year unless lawmakers act to restore the enhancements.
For many Arkansans, that sticker shock is already hitting. Here are some photos of real Arkansans’ premium increases:
Ashley, a mother of three, saw her premium increase from $62.02 to $404.49.
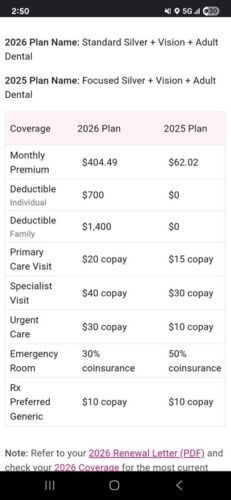
Leslie, her husband, and son’s premium increased from $19.54 to $3,391.72.
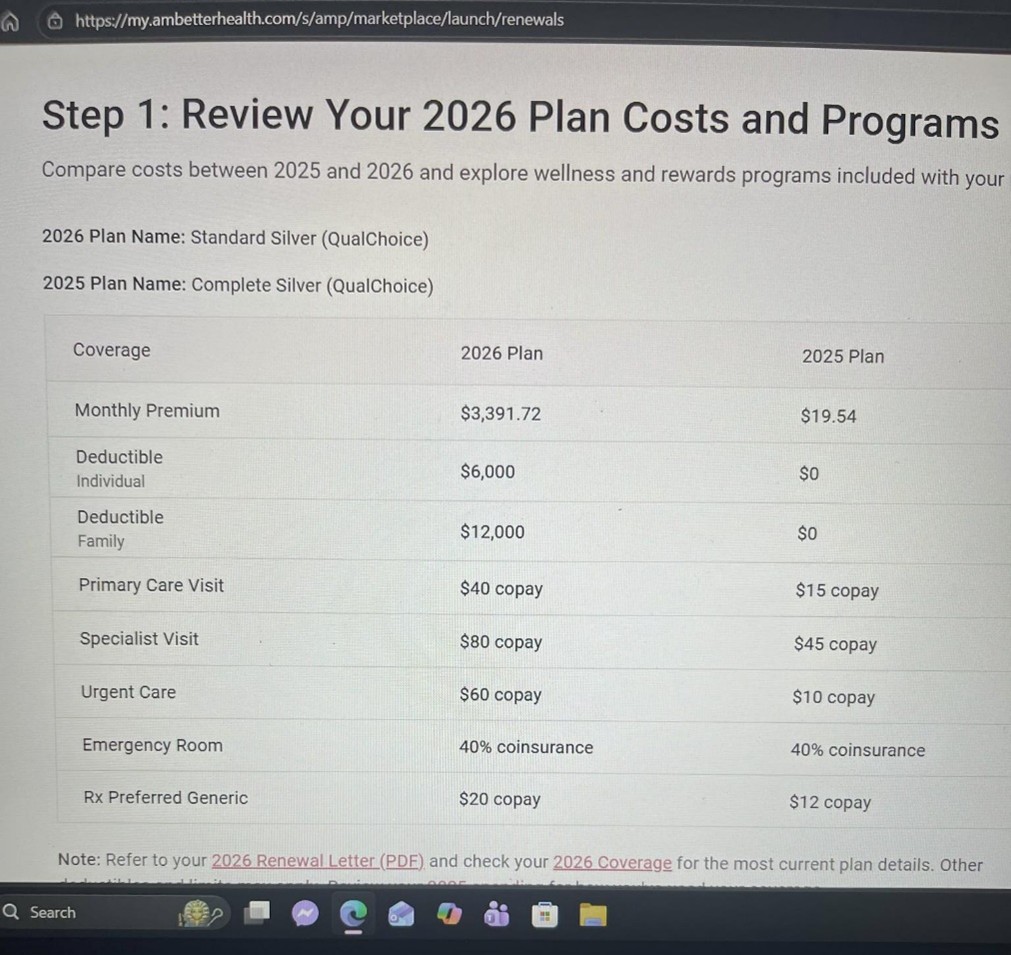
Stacy, a mother of a young child, saw her premium rise from $65.48 to $404.30.
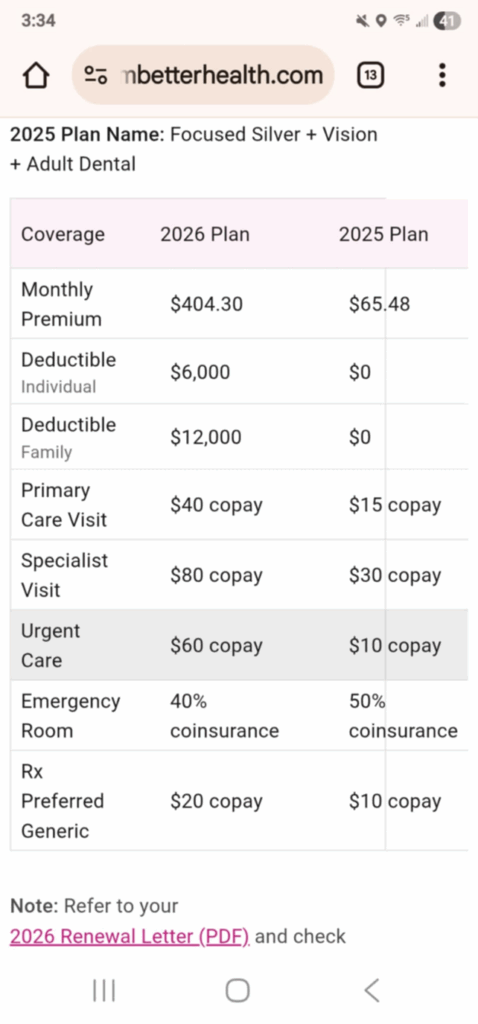
What Is in H.R. 1 and Why It Matters
H.R. 1 is a sweeping law passed over the summer. Among many provisions, it will affect the health insurance marketplace by:
- Raising costs for more than 22 million marketplace enrollees by allowing the enhanced premium tax credits to expire.
- Adding new paperwork and verification steps in Medicaid and the marketplace, creating more red tape for families.
- Making certain lawfully present immigrants ineligible for Medicaid, CHIP, or marketplace coverage.
- Ending the year-round enrollment opportunity for low-income adults under 150 percent of the federal poverty level.
- Removing the caps on how much people may have to repay if they receive more Advance Premium Tax Credit than they should.
- Allowing insurers to require people to pay back old premium debt before they can enroll again.
For Arkansas, the stakes are high. An estimated 131,000 people in the state are expected to lose coverage across Medicaid and the marketplace unless something changes.
What Marketplace Enrollees Should Expect This Fall
Here is what you should be watching for:
1. Notices from the marketplace and insurance companies
People should receive notices this fall, but many of them may not include actual 2026 premium tax credit amounts. That makes it much harder to tell what your real monthly bill will be until you actively shop for plans.
Half of marketplace enrollees are automatically re-enrolled every year. This year, that could mean not realizing your premium has increased until the January bill arrives.
2. Much higher premiums for many people
Without the enhanced premium tax credits, net premiums are expected to rise more than 75% on average. Many Arkansans are already seeing those numbers during plan previews.
3. More verification and paperwork
H.R. 1 includes new verification requirements and shorter deadlines to respond to data checks. Missing a notice could mean losing coverage.
4. Big potential tax bills
Starting in 2026, people who underestimate their income will owe back all excess premium tax credits. A change in job, hours, marital status, or disability status could lead to hundreds or thousands owed at tax time in 2027.
What People With Marketplace Coverage Can Do Right Now
1. Do not auto-enroll this year. Actively compare plans.
Go to HealthCare.gov and update your information. Even if you like your plan, your premium for next year may be very different.
2. Watch your mail and your online marketplace account.
Respond quickly to any requests for verification.
3. Reconcile Advance Premium Tax Credits when filing 2026 taxes.
This will be especially important next year to avoid losing future coverage.
4. Remember you can switch plans in January.
If you are auto-enrolled on November 1 and discover your plan is too expensive, you have until the end of January to choose a new plan for February.
5. Seek help if you need it.
Navigator organizations and community health centers can help you understand your options and complete enrollment. Check out HealthCare.gov/localhelp for assistance in your area.
What Individuals and Community Organizations Can Do
- Share information with clients, partner organizations, schools, and local media.
- Remind people that premiums may look very different this year.
- Connect people who remain uninsured to low-cost community care.
- Share examples of premium increases or losses of coverage. These stories help illustrate the impact in Arkansas.
- Contact your elected officials and ask them to extend the premium tax credit enhancements when the budget process continues. Remind them that Arkansas families deserve affordable health care.
